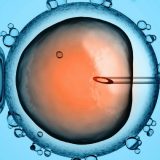
Today, many couples who wish to have a child may experience difficulties achieving pregnancy naturally. Infertility (sterility) can arise from various causes, and in such cases, in vitro fertilization (IVF) becomes an important option that offers hope for having a baby. Below are the conditions and patients for whom IVF treatment is applied:
1. Patients Who Have Undergone Ovarian Surgery
Conditions such as ovarian cysts, cancer, or endometrioma may reduce ovarian reserve and decrease the chances of natural conception. After such surgeries, IVF treatment can be an option to restore ovarian function.
2. Patients with Blocked or Removed Fallopian Tubes
Patients whose fallopian tubes are blocked or removed due to infections or ectopic pregnancy may have difficulty conceiving naturally. IVF offers an alternative by enabling fertilization outside the body.
3. Intra-Abdominal Adhesions
Previous abdominal surgeries, infections, or conditions such as endometriosis may cause adhesions, preventing communication between the ovaries and fallopian tubes. IVF can help overcome these barriers.
4. Patients with Ovulation Disorders
Women with ovulation problems, such as polycystic ovary syndrome (PCOS), may not ovulate regularly. IVF treatment can stimulate the ovaries appropriately and increase the chances of pregnancy.
5. Advanced Maternal Age
As women age, both the quality and quantity of eggs decline, reducing the likelihood of natural conception. IVF can be an effective option for stimulating the ovaries and obtaining healthy embryos.
6. Unexplained Infertility
Patients who cannot conceive despite thorough evaluation showing no identifiable issue are diagnosed with unexplained infertility. IVF may provide a solution in such cases.
7. Sexual Dysfunction
Conditions such as vaginismus in women or ejaculation disorders in men may make natural conception difficult. IVF can help overcome these obstacles.
8. Male Factor Infertility
Men with low sperm count, poor motility, or abnormal morphology may have reduced chances of natural conception. IVF can increase success rates by selecting healthy sperm and achieving fertilization in a laboratory setting.
9. Oncology Patients
Men who have undergone surgery due to testicular tumors or received cancer treatment may lose their fertility. IVF can be used with previously frozen sperm samples.
10. Congenital or Acquired Obstruction of Sperm Ducts
Men with congenital or acquired blockages in sperm ducts may face difficulty in natural conception. IVF can retrieve sperm directly from the testes to increase the chances of pregnancy.
11. Genetic Disorders
Couples at risk of genetic conditions can benefit from IVF combined with genetic testing to select healthy embryos and reduce the risk of hereditary diseases.
Before recommending IVF treatment, each patient should undergo a detailed evaluation, and the treatment plan should be individualized. The success of IVF depends on various factors such as the expertise of the clinic, technological infrastructure, and the health conditions of the couple.
NOVAART IVF Center in Ankara provides personalized and effective treatment options for couples experiencing infertility, guided by the most up-to-date scientific knowledge and supported by experienced IVF specialists.
What is IVF Treatment?
IVF treatment is a reproductive technology developed for couples experiencing infertility. Its main goal is to help couples who cannot conceive naturally.
In IVF treatment, the woman’s ovaries are stimulated with appropriate medications to produce multiple eggs. These eggs are then collected through a minor surgical procedure. Fertilization is carried out in a laboratory environment using sperm obtained from the male partner (the ICSI method may be used). The resulting embryos are then transferred into the woman’s uterus to initiate pregnancy.
IVF can be applied in various infertility cases, including blocked or removed fallopian tubes, diminished ovarian reserve, male factor infertility, sexual dysfunction, or unexplained infertility. The treatment process is usually planned as a cycle, and success rates may vary depending on several factors.
IVF is considered one of the major advancements in modern reproductive medicine and has enabled millions of couples to have children.
What Are the Advantages and Risks of IVF Treatment?
Advantages:
-
Opportunity to Have a Baby: Offers a chance of parenthood to couples who cannot conceive naturally.
-
Solution for Various Infertility Causes: Applicable to a wide range of infertility conditions.
-
High Success Rates: With technological advancements and expertise, success rates continue to improve.
-
Embryo Selection: Genetic testing allows for the selection of healthy embryos, reducing the risk of hereditary diseases.
-
Patient Control: Some stages of the treatment, such as ovarian stimulation, can be managed at home.
Risks and Disadvantages:
-
Multiple Pregnancy Risk: Transferring more than one embryo may increase the risk of multiple pregnancies, which can lead to complications.
-
Side Effects: Medications used for ovarian stimulation may cause side effects such as headaches, bloating, and emotional fluctuations.
-
Embryo Development Issues: There is a possibility that embryos may not develop as expected in the laboratory.
-
Cost: IVF treatment can be expensive and may create a financial burden for couples.
-
Psychological Impact: The process can be long and emotionally challenging, especially in cases of unsuccessful attempts.
The success and risks of IVF treatment vary depending on factors such as the experience of the clinic, the health status of the couple, and age. Therefore, a thorough evaluation and consultation before starting treatment are essential.