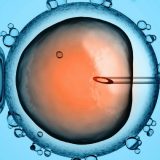
Although male infertility can be a significant obstacle for couples who wish to have a child, in vitro fertilization (IVF) offers an effective solution to overcome this challenge. Thanks to modern reproductive technologies, successful outcomes can also be achieved in cases related to male infertility. In this article, we discuss how IVF treatment is applied in male infertility cases, the methods used during the process, and the factors that increase the chances of success.
The Role of IVF Treatment in Male Infertility
In cases of male infertility, IVF treatment is especially preferred when sperm count is insufficient or sperm quality is low. Even when natural conception is not possible, this treatment significantly increases a couple’s chances of having a baby.
During IVF treatment, specialized techniques tailored to male infertility are used. These range from supportive methods aimed at improving sperm quality and quantity to advanced technologies such as intracytoplasmic sperm injection (ICSI).

Methods Used in IVF Treatment
1. Intracytoplasmic Sperm Injection (ICSI)
ICSI is one of the most commonly used methods to overcome male infertility in IVF treatment. In this technique:
-
A single healthy sperm is directly injected into an egg under a microscope.
-
It is successfully used in cases of low sperm count, poor motility, or abnormal sperm morphology.
2. TESA / PESA / MESA Methods
In men who produce sperm but have no sperm present in the ejaculate, sperm can be surgically retrieved from the testes or epididymis.
-
TESA (Testicular Sperm Aspiration): Sperm is collected from testicular tissue using a needle.
-
PESA (Percutaneous Epididymal Sperm Aspiration): Sperm is obtained from the epididymis.
-
MESA (Microsurgical Epididymal Sperm Aspiration): Sperm is retrieved through a more detailed microsurgical procedure.
3. Use of Donor Sperm
If sperm cannot be obtained from the male partner, the use of donor sperm may be considered as an alternative. This option is applied in rare cases where genetic material cannot be provided.
The IVF Process: Step by Step
Evaluation and Preparation
Both partners undergo a comprehensive evaluation. When male infertility is diagnosed, the most appropriate treatment method is determined. Semen analysis and genetic tests play a crucial role at this stage.
Ovarian Stimulation
Hormonal treatment is administered to the woman to stimulate the ovaries and enable the production of multiple eggs, increasing the chances of fertilization.
Sperm Collection and Processing
The sperm sample obtained from the male partner is processed in the laboratory using specialized techniques. In cases of very low sperm count, sperm may be collected through surgical methods.
Fertilization and Embryo Development
Using the ICSI technique, sperm is directly injected into the egg, and embryo development is monitored in the laboratory.
Embryo Transfer
The healthiest developing embryos are selected and transferred into the woman’s uterus. After this stage, the pregnancy test is awaited.
Factors That Increase the Chance of Success
Several key factors influence the success of IVF treatment in cases of male infertility:
-
Sperm Quality: If no genetic or structural abnormalities are detected in sperm analysis, success rates increase.
-
Female Age: The woman’s age and ovarian reserve directly affect IVF success.
-
Expertise and Technology: Receiving treatment at a center with an experienced team and advanced technology significantly improves success rates.
-
Lifestyle: Adopting a healthy lifestyle contributes positively to the treatment process.
Psychological Support: An Essential Part of the Process
IVF treatment can be physically and emotionally demanding for couples. Therefore:
-
Couples supporting each other throughout the process,
-
Seeking professional help for stress management,
-
Maintaining continuous communication with the specialist doctor and medical team
are all extremely important.
Conclusion: There Is a Solution, There Is Hope
Thanks to the possibilities offered by modern medicine, male infertility is no longer an insurmountable obstacle. IVF treatment has helped countless couples achieve their dreams of parenthood.
At Novaart, we are here to guide you through this journey and provide the support you need. For more detailed information and personalized solutions, feel free to contact us.